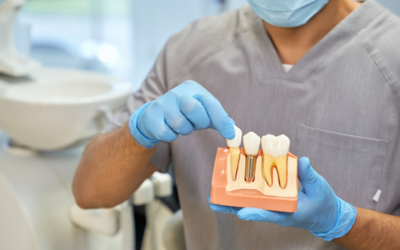
When you need to replace a tooth, there is no better option than a dental implant. Not only do dental implants provide unmatched strength and support, but they also offer an incredible success rate estimated to be as high as 95%.[1] However, that doesn’t mean there’s no potential for complications.
On the off chance that you do experience complications with your dental implants, it would be both valuable and reassuring to understand what to expect and how to manage any issues that may arise. To help you do that, look at this quick and easy guide to one of the more well-known dental implant complications: peri-implantitis.
What Is Peri-Implantitis?
Peri-implantitis is an inflammation of the gum tissue that can occur around a dental implant. This issue can also be paired with the deterioration of the jawbone, which supports the implant.[2] This issue is like periodontal disease in that it affects the gum tissue, involves bacterial buildup, and is most commonly caused by poor oral hygiene.
Like periodontitis, this infection occurs in multiple stages. It begins with simple inflammation and, if left unchecked, can continue developing into more severe inflammation and bone loss. Eventually, it can progress into advanced peri-implantitis, at which point symptoms become severe, infection can occur, and the implant can ultimately fail.
Signs You May Have Peri-Implantitis
It’s essential to catch peri-implantitis early on to avoid more severe symptoms and complicated treatments. To do that, keep an eye out for the following:
- Redness and inflammation of the gum tissue
- Tenderness or pain around the area of the implant
- Bleeding gums
- Bad breath
- Painful chewing or speaking
Later stages of peri-implantitis can be identified by a bad taste in your mouth, pus around the implant site, and even a loosening of the dental implant. If you’re experiencing any of these, contact an emergency periodontist immediately. These symptoms generally signify an infection that can be serious.
Common Causes of Peri-Implantitis
While the most common reason for peri-implantitis is a poor oral hygiene routine that allows bacterial buildup and infection, some other factors can significantly raise your risk. Those factors include the following:
Smoking
Smoking also decreases blood flow and reduces the function of the immune system to fight infections. (not to mention it causes more plaque to build up), all of which can result in a higher risk for infection. When your periodontist urges you to avoid smoking altogether, this is one of the significant reasons.
Insufficient Bone Mass
If an implant is placed without enough bone mass to support it, the risk of infection becomes elevated. Bone grafts may be necessary to avoid this issue.
Diabetes
Lack of proper blood flow due to diabetes can increase the chance of infection occurring, and it can also make it far more challenging to heal from the infection once it has occurred.
Compromised Immune Systems
If your immune system is compromised, you may struggle to fight off infection. This can result in not only a higher risk for peri-implantitis but also the potential for the infection to be worse.
Diabetes
Lack of proper blood flow due to diabetes can increase the chance of infection occurring, and it can also make it far more challenging to heal from the infection once it has occurred.
Foods
Certain foods, like popcorn, may cause a local inflammatory reaction, which can lead to peri-implantitis and loss of bone around the implant.
Avoiding Dental Care
You should see your periodontist regularly to ensure your oral health and keep an eye on your dental implant. Avoiding appointments can allow a minor issue to develop into a larger one, leaving you with peri-implantitis to deal with.
Treating Peri-Implantitis With Rochester Periodontics and Implants Services
If you develop peri-implantitis, treatment will depend on the severity of the infection and the nature of the symptoms. In general, you can anticipate that your periodontist will suggest one or more of the following treatments:
Chlorhexidine Mouthwash
The first form of treatment is a special mouthwash that can help to kill off the bacteria causing the infection. There are also special antimicrobial gels that your periodontist may prescribe.
Antibiotics
An antibiotic can also be prescribed to help eliminate some of the infection-causing bacteria before surgical intervention is deemed necessary.
Debridement
Your periodontist may also use specialized tools to access the area around the implant to remove plaque and tartar contributing to the infection.
Surgical Procedures
If the infection is too significant for non-surgical approaches, then a few surgical options can help address the issue. These procedures can work to remove infected tissue, regenerate lost bone mass, and manage the infection with the help of antimicrobials.
Rochester Periodontics and Implants Services
If you’re looking for Rochester periodontics and implants, contact Dental Implants & Periodontal Health of Rochester. Dental implants are the best option available when it comes to tooth replacement. Call us at 585-685-2005 or go online to schedule an appointment today.
Sources: